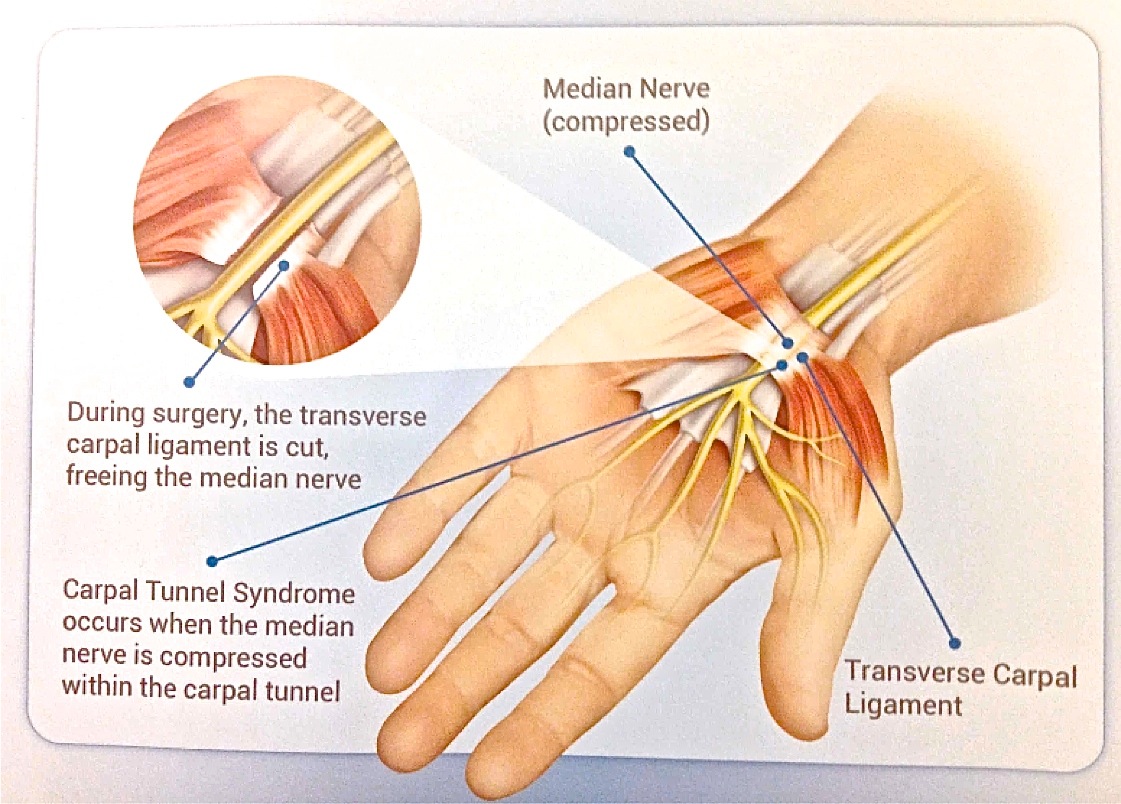
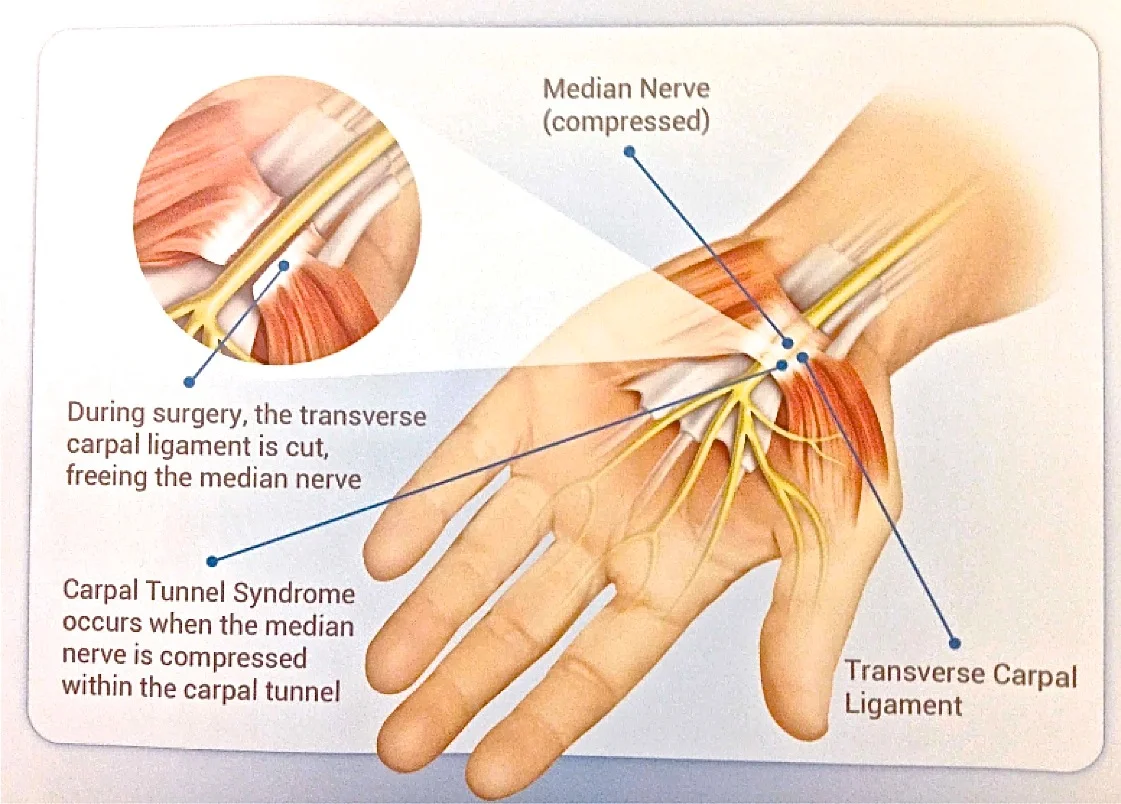
Physical Therapy for Carpal Tunnel Syndrome
/Carpal tunnel syndrome is a painful disorder that affects millions of Americans annually. Although some individuals may feel pain in the wrist and hand from the carpal tunnel syndrome, discomfort can also radiate throughout the entire arm. To successfully treat carpal tunnel syndrome, patients can attend regular physical therapy sessions. In fact, according to a study published in “The Journal of Pain,” physical therapy was found to improve function and pain as effectively as surgical options (Fernández-de-Las Peñas, Ortega-Santiago, de la Llave-Rincón, Martínez-Perez, Fahandezh-Saddi Díaz, Martínez-Martín, Pareja,Cuadrado-Pérez 2015). During the study, participants went to three 30-minute PT sessions weekly and a single educational session on home and work remedies. After one month in the study, a significant reduction in pain levels were reported.
Flexibility exercises for carpal tunnel
One potential way a physical therapist can treat carpal tunnel sufferers is by guiding them through a series of flexibility exercises for the wrist and hand. Flexing and moving different muscle groups within the hand can alleviate symptoms. For instance, a physical therapist can demonstrate to the patient how to stretch out the palmar fascia and the median nerve—two of the areas irritated because of carpal tunnel syndrome. There are deep stretches that work the flexor muscles in the hand and will prevent issues from cropping up such as tightness in the affected hand at night. Regular intervals of stretching are also useful for preventing the nightly cramping typically experienced by carpal tunnel patients.
Rest Periods
In conjunction with the exercises, a physical therapist is likely to recommend periods of rest for the patient. By limiting movement for two to six weeks, inflammation will alleviate and stop pressing against the nerve. To keep the wrist immobilized, the patient can wear a splint. The split doesn’t normally need to be worn around the clock, but instead put on at night.
Hot/cold therapies
A physical therapist can present carpal tunnel patients with the option of doing contrast hydrotherapy. This alternative remedy is effective at not only giving pain relief, but also getting rid of inflammation and promoting the body’s natural healing process. During a session, the affected hand and wrist can be immersed in warm water for several minutes followed by a shorter interval of cold-water exposure.
Posture
Although posture doesn’t seem like it would directly affect carpal tunnel syndrome, good posture is extremely important. Since carpal tunnel syndrome is more common in individuals who perform repetitive tasks, like typing, a physical therapist is likely to stress the importance of taking frequent breaks and practicing good posture while on the job. A physical therapist can recommend the following best practices for good posture:
- Relaxed shoulders
- Spine flush against the back of desk chair
- Elbows at rest against sides
- Wrists straightened out
- Feet firmly on floor
- Eyes level
For patients who are unsure the root cause of their carpal tunnel syndrome, the physical therapists may recommend an on-site assessment. The therapist can visit the workspace and make suggestions on how to avoid aggravating the carpal tunnel symptoms.
Anti-vibration tools
Many workers are exposed to a phenomenon called hand arm vibration syndrome (HAVS). Those who use hand tools frequently as part of their occupation are more prone to having issues such as carpal tunnel syndrome and Raynaud’s. A physical therapist could introduce tools like the anti-vibration glove to combat this issue. During use, the gloves reduce the amount of vibration experienced by the wearer.
Although physical therapy is an important part of carpal tunnel treatment, a therapist is also invaluable for post-surgery care. As the patient recovers from corrective surgery, he or she will need help regaining strength and movement in the hand and wrist. The therapist can also act as an educational resource to explain how to take preventive measures to avoid nerve compression in the future. Patients are urged to take frequent movement breaks throughout the day and become aware of how changing wrist positions recurrently will help their condition.